Employees struggling with fertility challenges often express concerns that treatment could impact their career prospects and affect their productivity at work.
To help juggle workplace commitments alongside medical appointments, Fertility Network UK is encouraging IVF clinics to become more responsive to patients’ constraints and is launching a ‘Clinic Pledge’ as part of its ‘Fertility in the Workplace’ initiative.
Little support at work
In a recent survey of fertility patients conducted by Fertifa and Fertility Network UK (2023), 75% of those interviewed said their productivity at work was strongly impacted by fertility challenges, and more than a third (37%) said that they received very little or no support from their employer. A CIPD (2023) survey found that 40% of employers don’t have a fertility policy and don’t plan to introduce one, leaving those impacted by this medical condition feeling unsupported, isolated and in fear of discrimination.
Claire Heuclin of Fertility Network UK (pictured) comments: “Our Fertility in the Workplace initiative already offers guidance and support to employers who are looking to understand more about fertility and improve workplace support and education for their staff, as well as providing free support to the one in six affected by infertility struggles, all of whom are of working age.
“Now we are proud to announce our new initiative specifically for clinics and their patients. As the UK’s leading patient-led fertility charity, along with the expertise from Bourn Hall Clinic, we can provide insights to clinics based on patient experiences and offer recommendations on how they can become more supportive of their own patients as they navigate their fertility journey alongside workplace commitments.”
The ‘Clinic Pledge’ asks fertility centres to:
- Raise awareness of Fertility in the Workplace support services by signposting patients to online resources containing tools and information to build their confidence in starting a conversation with employers. (There are also training resources for employers to use with their teams to better understand the impacts of infertility and treatment.)
- Consider small operational changes, such as offering online appointments and a choice of communication methods to help patients work around their own workplace constraints.
- Demonstrate best practice by implementing a fertility policy in the clinic and subscribing to employer workplace support and education packages. This includes recognition of the needs of staff members who may be experiencing their own fertility challenges in what can be a very triggering working environment.
Bourn Hall shares experiences and templates
Fertility in the Workplace is supported by the VCSE Health and Wellbeing Fund and Bourn Hall, the world’s first IVF clinic, and is delivered by Fertility Network UK. In collaboration with Bourn Hall, a ‘tool kit’ has been developed that includes templates as starting points for other clinics to develop bespoke fertility policies and workplace focussed patient information.
Dr Thanos Papathanasiou, CEO and Medical Director of Bourn Hall, says: “We believe that a more flexible approach will benefit both patients and clinics. It will reduce the stress, particularly for patients who have restrictive work patterns, such as teachers and shift workers, and improve the patient experience and their ability to access treatment.
“We are delighted to pioneer this initiative with Fertility Network UK and to share our experiences with others to promote best practice.”
Claire Heuclin continues: “We would welcome feedback from patients and their clinics about what works well. We are determined to create a lasting change in workplace culture to make it more supportive for those struggling with fertility challenges.”
More information
More information about Fertility in the Workplace and the Clinic Pledge is available at bit.ly/FiTWsupport
If you have any thoughts or feedback on your own experiences, or are looking for 1:1 support or guidance as an employee, please contact the Fertility in the Workplace team via [email protected] (all feedback will be handled entirely anonymously unless otherwise agreed).























 Megan Jolly, from Swaffham, Norfolk said that she had never heard about endometriosis until the couple started trying for a baby.
Megan Jolly, from Swaffham, Norfolk said that she had never heard about endometriosis until the couple started trying for a baby.


 “We had our embryo transfer at Easter and Louis was born on Christmas Day. It was very bizarre how it worked out that way! He is truly a little miracle.”
“We had our embryo transfer at Easter and Louis was born on Christmas Day. It was very bizarre how it worked out that way! He is truly a little miracle.”












 Lyla is now a “lovely, sassy, chatty girl” says her proud mum. She will be celebrating her first birthday at home surrounded by friends and family.
Lyla is now a “lovely, sassy, chatty girl” says her proud mum. She will be celebrating her first birthday at home surrounded by friends and family.








 Dr Mike Macnamee, CEO of Bourn Hall, explains the significance of Jean’s role as an embryologist: “Jean was a nurse in Cambridge before accepting the opportunity to work with Professor Edwards at the University. Edwards had a breakthrough in 1969, when the first human egg fertilised outside of the body survived for five days, reaching blastocyst stage. This showed that IVF was possible.
Dr Mike Macnamee, CEO of Bourn Hall, explains the significance of Jean’s role as an embryologist: “Jean was a nurse in Cambridge before accepting the opportunity to work with Professor Edwards at the University. Edwards had a breakthrough in 1969, when the first human egg fertilised outside of the body survived for five days, reaching blastocyst stage. This showed that IVF was possible.
 Louise Brown comments: “This is a very special day. I’m just so glad Jean Purdy is finally getting the recognition she deserves; it is what Bob and Patrick always wanted. My mum always said it’s not just about the babies being born; it is about creating families. Without IVF she wouldn’t have had me or my sister or her grandchildren.”
Louise Brown comments: “This is a very special day. I’m just so glad Jean Purdy is finally getting the recognition she deserves; it is what Bob and Patrick always wanted. My mum always said it’s not just about the babies being born; it is about creating families. Without IVF she wouldn’t have had me or my sister or her grandchildren.” Angela Roberts from Bedfordshire had successful treatment in 1990 and is now a grandma. Nikki’s daughter Cleo was conceived at Bourn Hall with IUI. Angela says: “If it hadn’t been for IVF, my girls wouldn’t be here, and nor would Cleo be here. It’s an absolutely wonderful thing”
Angela Roberts from Bedfordshire had successful treatment in 1990 and is now a grandma. Nikki’s daughter Cleo was conceived at Bourn Hall with IUI. Angela says: “If it hadn’t been for IVF, my girls wouldn’t be here, and nor would Cleo be here. It’s an absolutely wonderful thing” Angeliqua Smith from Luton has PCOS, a common cause of female infertility that causes irregular ovulation. She came with her mum and baby daughter, Isabella. “It is magical being a mum,” says Angeliqua. “There is so much frequent joy in everyday moments, when she says a new word or starts laughing or smiling or just does something completely unexpected. It is just lovely doing things together with her.”
Angeliqua Smith from Luton has PCOS, a common cause of female infertility that causes irregular ovulation. She came with her mum and baby daughter, Isabella. “It is magical being a mum,” says Angeliqua. “There is so much frequent joy in everyday moments, when she says a new word or starts laughing or smiling or just does something completely unexpected. It is just lovely doing things together with her.” Claire and Alex Martin from Hitchin came with their son Robin, who was conceived after treatment for male infertility. “To us, IVF means hope,” says Claire. “When Robin was born, and he was put on my chest I just burst into tears. We both looked at him and said, ‘we have been waiting so long for you!’ He was so beautiful.”
Claire and Alex Martin from Hitchin came with their son Robin, who was conceived after treatment for male infertility. “To us, IVF means hope,” says Claire. “When Robin was born, and he was put on my chest I just burst into tears. We both looked at him and said, ‘we have been waiting so long for you!’ He was so beautiful.”


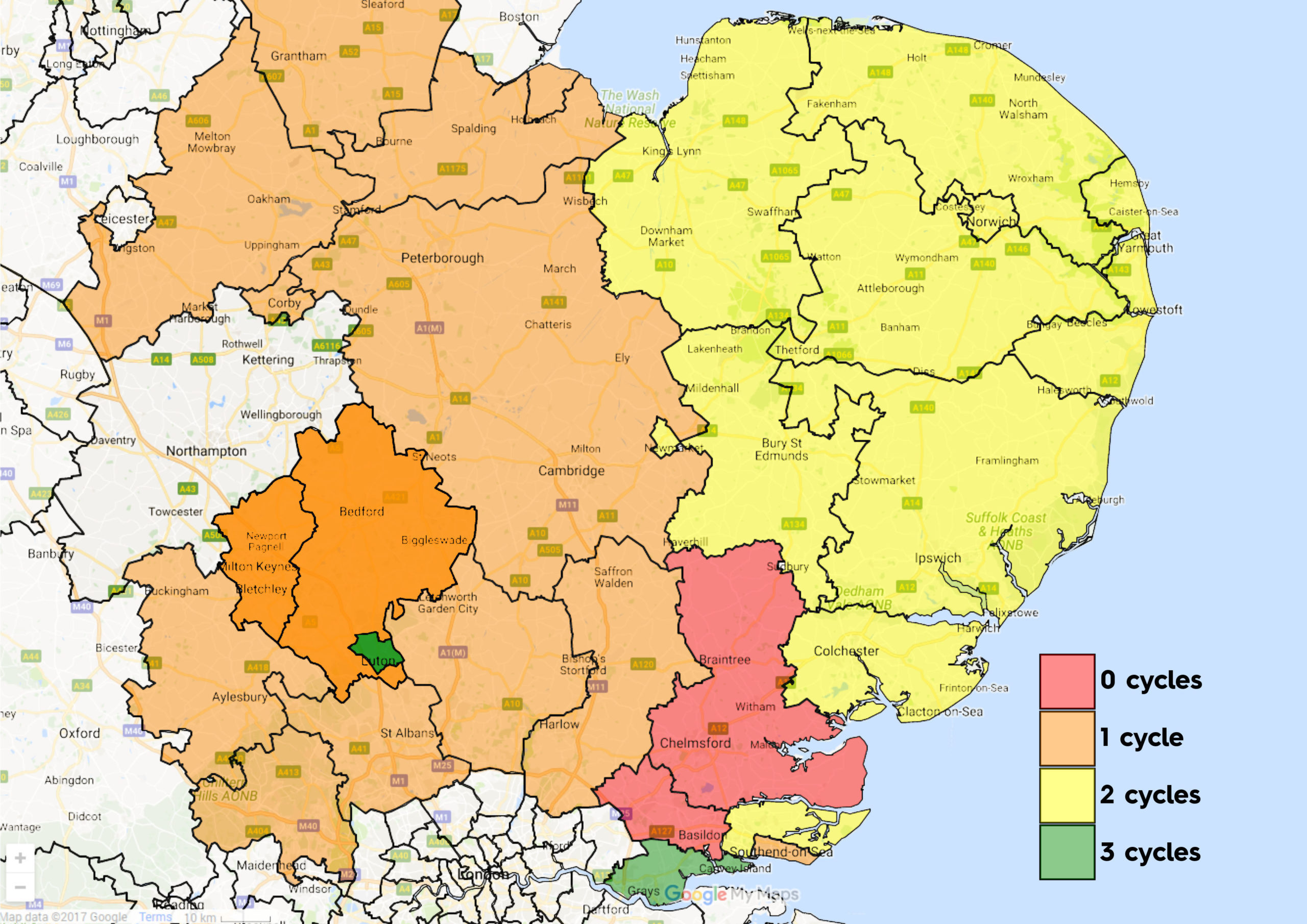
 Fertility Network UK is urging family and friends of people struggling with infertility – and seen the impact on their lives – to participate in a consultation (closing 21st December) on NHS funded-IVF treatment across Luton, Bedfordshire and Milton Keynes. Only Luton offers the recommended three cycles of treatment and local commissioners want to cut this so that all areas have just one.
Fertility Network UK is urging family and friends of people struggling with infertility – and seen the impact on their lives – to participate in a consultation (closing 21st December) on NHS funded-IVF treatment across Luton, Bedfordshire and Milton Keynes. Only Luton offers the recommended three cycles of treatment and local commissioners want to cut this so that all areas have just one.









 Speaking ahead of Father’s Day, and now a proud dad to one-year-old son Hendrix, Dan, aged 33, says: “Being a Dad is something that I had always wanted but as time went on thought might never happen.”
Speaking ahead of Father’s Day, and now a proud dad to one-year-old son Hendrix, Dan, aged 33, says: “Being a Dad is something that I had always wanted but as time went on thought might never happen.”
































 The new purpose-built clinic at Wickford will have the capacity for 1,000 IVF cycles a year. It is built to the highest environmental specifications, incorporating the latest building technologies to reduce noise and vibrations from traffic to create a calm interior.
The new purpose-built clinic at Wickford will have the capacity for 1,000 IVF cycles a year. It is built to the highest environmental specifications, incorporating the latest building technologies to reduce noise and vibrations from traffic to create a calm interior.
 The couple were treated at Bourn Hall Clinic using a procedure called ICSI (intracytoplasmic sperm injection), where a single sperm is injected into an egg to fertilise it. Two weeks later Victoria discovered she was pregnant.
The couple were treated at Bourn Hall Clinic using a procedure called ICSI (intracytoplasmic sperm injection), where a single sperm is injected into an egg to fertilise it. Two weeks later Victoria discovered she was pregnant.










 So we carried on across the expanse of the great frozen plateau. For 16 days we went on and on with little sign of the terrain giving us any respite, until finally we saw the Trans-Antarctic Mountains. What a sight! We were full of hope, full of hope that we’d start descending to a better place, where the temperature was more survivable, the air’s easier to breathe, and the ice would just glide us downhill.
So we carried on across the expanse of the great frozen plateau. For 16 days we went on and on with little sign of the terrain giving us any respite, until finally we saw the Trans-Antarctic Mountains. What a sight! We were full of hope, full of hope that we’d start descending to a better place, where the temperature was more survivable, the air’s easier to breathe, and the ice would just glide us downhill. As we camp now on the far side of Antarctica, waiting to be picked up, I share my joy with you at having been part of SPEAR17. And I must also give a huge thank you for all the support we’ve had following our expedition. It’s been really special for us to receive messages of support from you, and to hear through Wendy that we’ve managed to share our journey with you as well. I’d like to say thank you to all our sponsors and to the British Army; you placed great faith in Lou and this expedition, and your backing made this all possible.
As we camp now on the far side of Antarctica, waiting to be picked up, I share my joy with you at having been part of SPEAR17. And I must also give a huge thank you for all the support we’ve had following our expedition. It’s been really special for us to receive messages of support from you, and to hear through Wendy that we’ve managed to share our journey with you as well. I’d like to say thank you to all our sponsors and to the British Army; you placed great faith in Lou and this expedition, and your backing made this all possible. There’s certainly some recovery to be done, and fortunately we have some time in Chile before we get back to the UK to give us that chance, that chance of at least looking like half the men we were when we left before we’re reunited with our families and our partners.
There’s certainly some recovery to be done, and fortunately we have some time in Chile before we get back to the UK to give us that chance, that chance of at least looking like half the men we were when we left before we’re reunited with our families and our partners.
