Breaking news IVF treatment: @ENHertsCCG (North and East Hertfordshire CCG) to drop to one cycle and @HVCCG (Herts Valley CCG) to drop to 0, to be reviewed in 12 months, according to Healthwatch Herts
We are waiting for an official announcement from the three CCGs who recently invited consultation on this decision (Herts Valley, East and North Herts and West Essex).
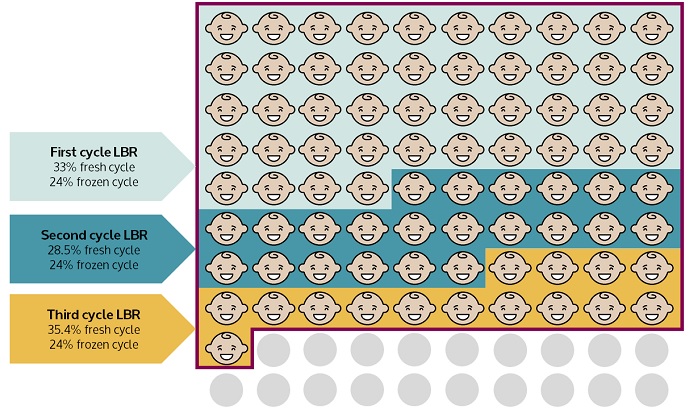
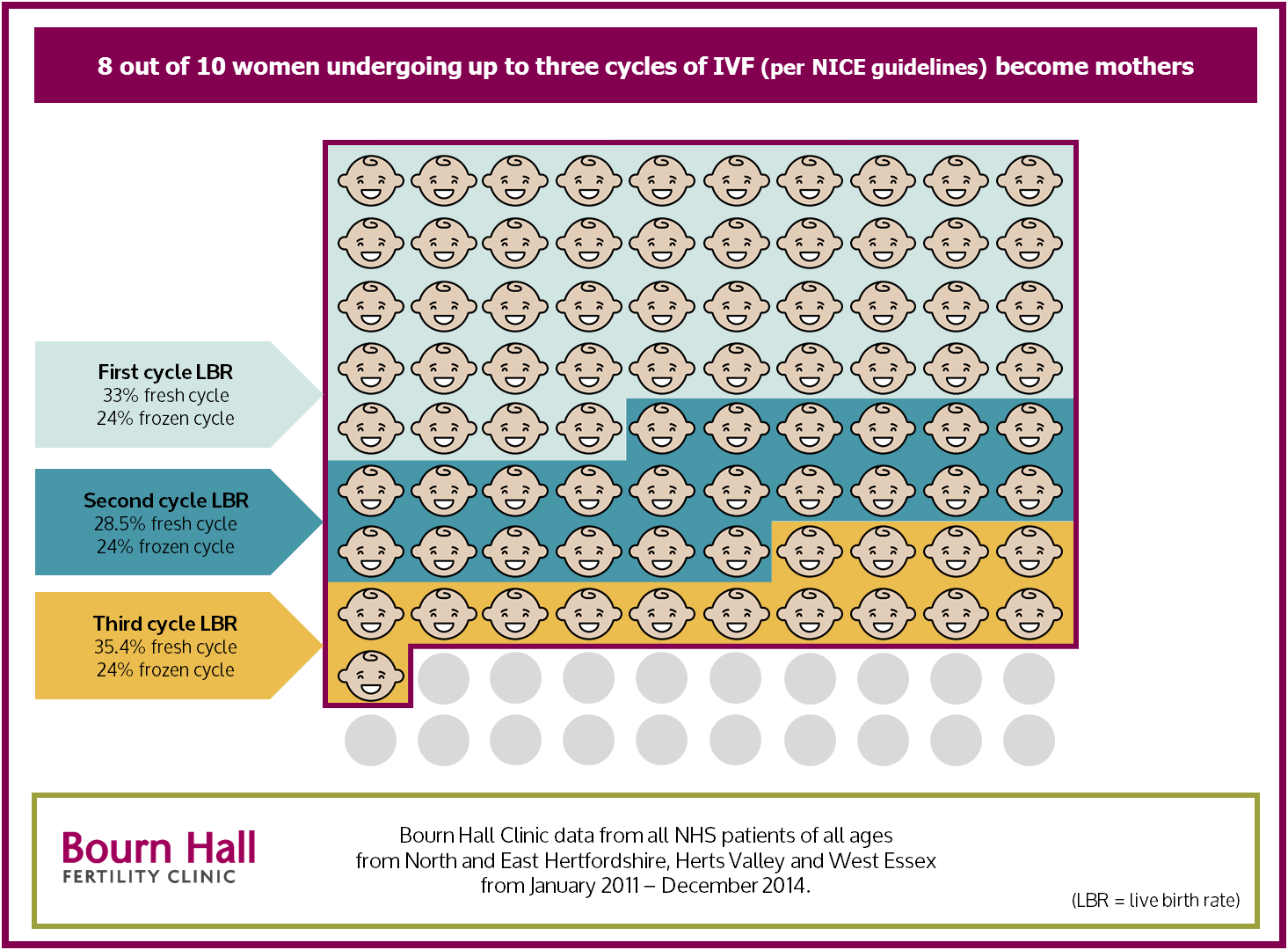
80 per cent of Herts IVF patients who meet the strict criteria will have a baby if they are given the option of three full cycles, the NICE (National Institute for Health and Care Excellence) recommendation. This information, based on the experience of real patients in Hertfordshire over 5 years, has not been used within a consultation document produced by the Clinical Commissioning Groups (CCGs) who cover Hertfordshire and West Essex.
The ‘Healthier Future Let’s Talk’ document1 has been produced by North and East Herts, Herts Valley and West Essex CCGs to inform a debate about cutting funding for specialist fertility treatment. It uses national data to suggest that if 100 women are given treatment “according to the NICE fertility guidance” only 20 – 35 will have a baby. The true figure for patients in the region who have had treatment at Bourn Hall is closer to 80 if they can have up to three cycles as recommended by NICE.
Between 2009 and 2014 all patients in Hertfordshire and Essex who met the criteria were entitled to three cycles of IVF as recommended by NICE2. During this time 33% of NHS couples became pregnant on their first cycle of IVF when treated at Bourn Hall. After three cycles this increases to 8 out of 10 women giving birth.
A more effective approach for fertility care
Dr Mike Macnamee is the CEO of Bourn Hall. He explains that when the clinic was awarded a five-year contract for NHS-funded IVF in 2009, it was able to improve treatment, drive down costs and increase success rates for Herts IVF patients.
He comments: “We have five years of real data about real patients that demonstrate clearly the benefits of implementing the NICE guidelines for those that meet the eligibility criteria.
“The CCG has not talked to us about how fertility care could be delivered more effectively. A more integrated approach that would involve GPs and fertility specialists working more closely together would streamline the system, create better outcomes and be more cost-effective for the CCGs.”
Success rates for IVF are highly individual. A healthy 27 year old woman with lots of eggs whose partner has a low sperm count may have a 50% chance of getting pregnant first time but the odds for an older woman who produces fewer eggs would be lower.
To make it easier for couples to calculate their chances of success after one or more cycles of treatment, researchers at the University of Aberdeen have created an online tool3. It uses a model that takes HFEA data for 113,873 couples and then adjusts it to take into account age, time spent trying to conceive, and type of infertility. Some may require IVF sooner while others may need more cycles of IVF treatment to become pregnant.
The study, led by David McLernon, and reported in the BMJ3, makes the point that using unadjusted data is not representative of the true chances of success.
The Hertfordshire and West Essex CCG consultation cites the BMJ paper as evidence but uses the unadjusted HFEA data to imply that for every 100 women who have IVF or specialist fertility treatment only 20 will have a baby as a result4. It neglects to say that this is based on one cycle and is not the accumulated success rate achieved by implementing the full NICE guidelines.
Furthermore it uses a different study to suggest that unsuccessful IVF treatment increases the chance of depression, despite the widely accepted understanding that it is infertility that causes severe mental distress.
Dr Macnamee continues: “Infertility is a medical condition and it deserves better diagnosis at an earlier stage.
“Recent cuts in funding have signalled that this area of medicine is not a priority and as a result the causes of infertility are also not being properly investigated. The risk is that even couples who might conceive naturally will miss out on having a baby as they are not being given relevant advice or medication.
“Withdrawal of funding will encourage people to go abroad for treatment and a few returning with multiple pregnancy will wipe out any saving.”
Herts IVF consultation
The consultation on IVF and specialist fertility services in the Hertfordshire and West Essex closes on the 14th September 2017 more information and the online questionnaire is available on www.healthierfuture.org.uk/ivf
- Consultation paper ‘A healthier future: Let’s Talk IVF and fertility services in Hertfordshire and west Essex’. http://www.healthierfuture.org.uk/publications lifts data from the BMJ paper but the diagram on page 7 neglects to say this is based on data from one cycle and not the NICE fertility guidelines as implied.
- In 2004 NICE produced clinical guidelines based on evidence. It recommended that 3 full cycles of IVF treatment should be provided to infertile couples, where the woman was aged 23-39, had an identified cause for their infertility or who had unexplained infertility for 3 years.
- Predict your personal success rate – This online tool developed by researchers at Aberdeen University is available here: http://w3.abdn.ac.uk/clsm/opis/home/about
- Predicting the chances of a live birth after one or more complete cycles of in vitro fertilisation: population based study of linked cycle data from 113 873 women. David J McLernon et al BMJ 2016;355:i5735 http://www.bmj.com/content/355/bmj.i5735/rapid-responses