Embryo transfer can be seen as it happens. Katy, 36, shares her experience.
Katy has a five-year-old son (conceived via a successful cycle of IVF with her former husband) but suffers from unexplained infertility. When she met her new partner J, who has no children of his own, she was very open about her wish to have more children and the fact she would probably need to have IVF again – and soon! Luckily that didn’t put him off – and they made an appointment at Bourn Hall’s Wickford clinic just a few months later ….
Getting to embryo transfer day was quite a nail-biting five days
“On the day of egg collection we were told there were five good eggs. Phew! (Although I would have loved to have got to double figures, if I’m being totally honest).
But it’s not until the next morning that you find out if any have fertilised. It’s not common that none fertilise. But it does happen, so obviously that plays on your mind.
Thankfully of the five, four had fertilised and they were “good” embryos which meant Bourn Hall were happy for us to aim to get to the blastocyst stage (so to wait another four days until embryo transfer.)”
Waiting for news
“It’s nerve-racking to think of them sitting there – hopefully cells dividing and growing – for four long days so we requested the clinic gave us a call to update us on day two and day three.”
This meant we knew when we arrived for embryo transfer that things were looking positive.

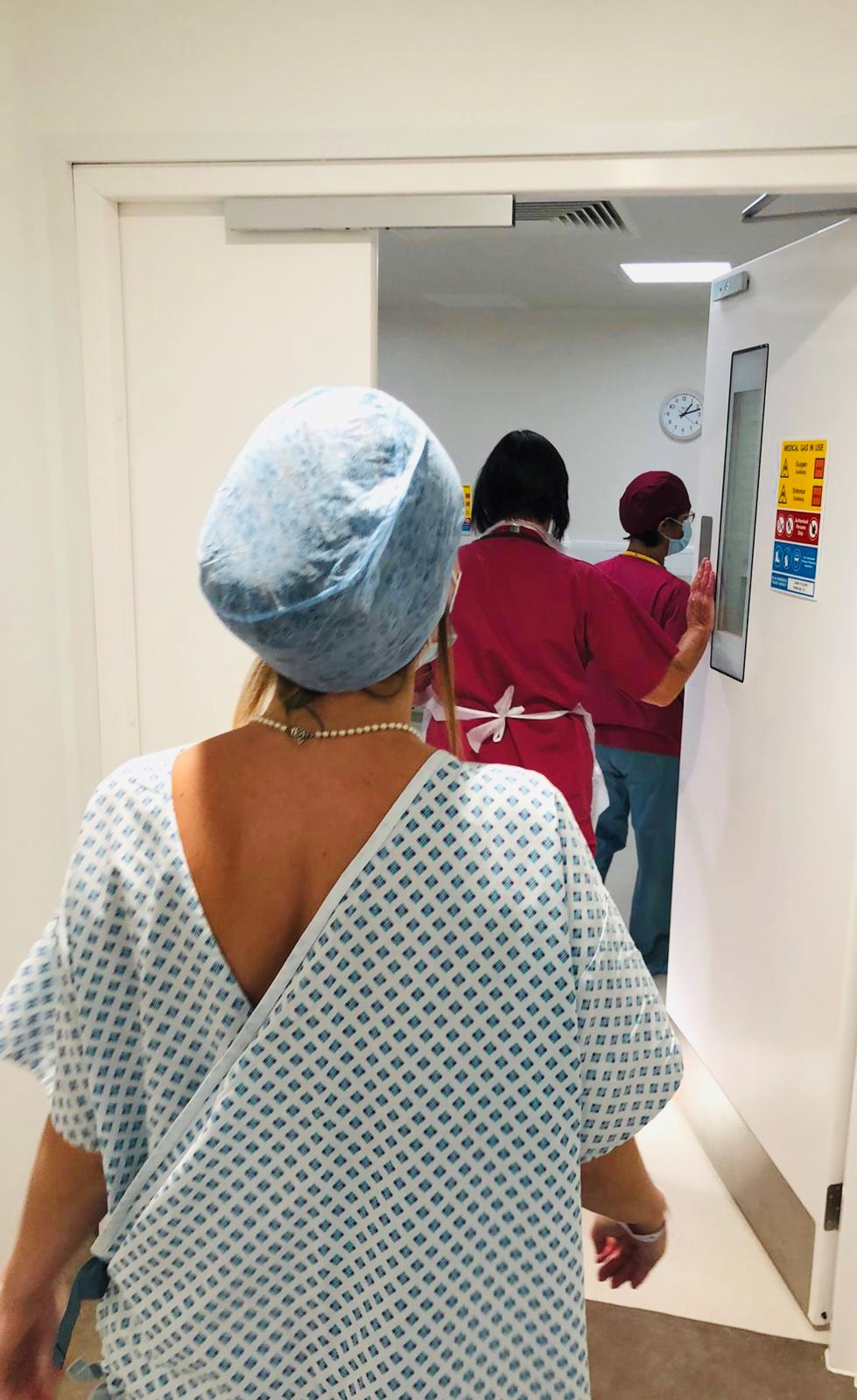
A decision to make
“As far as procedures go, the embryo transfer is a lot simpler and a whole lot quicker than egg collection.
Though it takes place in the same clinic, with a few of the same team, the atmosphere is very different.
Your partner can be with you. There’s no need for sedation. And you can watch everything that’s going on!
We were hoping we would be in a position to put one blastocyst back and be able to freeze one, maybe two.
As it happened, there were two that were good enough to be used. Unfortunately the second was not of good enough quality to freeze.
Sat there in my gown, we had a decision to make.
The odds of success with one blastocyst were about 45 per cent. The odds of success with two put back were 46 per cent. But if two were put back the odds of twins rocketed by at least 10 per cent.
It was a tough choice. But we opted for just the one, best quality blastocyst to go back.”
The action was screened
“As we watched, there was a little flash on the screen as our embryo (dubbed BB as that is the grading it was!) was transferred as close to the lining of my womb as it could be.
To aid the clarity of the picture on the screen, I needed to have a full bladder. This inevitably meant that throughout the whole process the most pressing thing on my mind was the fact I needed a wee.
But it’s the strangest of feelings walking out of the clinic (once finally having had a wee!) knowing that at that moment you have a perfect little embryo growing inside you. That at that moment you are actually two weeks pregnant. And from now on there’s really nothing you can do but wait and hope.” (And keep using your Crinone gels…)
Read more about Katy’s journey
Overview of the Fertility Journey
IVF down regulation bringing me down

Jackie Richardson, Lead Nurse at Bourn Hall Wickford, says:
During IVF treatment there is often a lot of discussion about embryo grading. This is an index used to help embryologists decide which embryo has the best chance of success and therefore which one should be transferred.
Patients should be reassured though that the grade of the embryo is not a way of predicting the health of the baby. We have seen many perfectly formed and healthy babies result from embryos that were classified as lower grade.







