Louise Brown’s birthday, 25th July, is World Embryologist Day. We talked to lead embryologist Adam Burnley about the changes he has seen since Bourn Hall, the world’s first IVF clinic, was established 40 years ago.
Although to be an embryologist you now need a life sciences degree and to have completed the Scientist Training Programme (STP) to enter the profession, when Adam Burnley started his career at Bourn Hall in 1986, the science was still developing.
“When I started at Bourn Hall, the pioneers of IVF, Patrick Steptoe and Bob Edwards, were still working at the clinic and their first ‘test tube’ baby Louise Brown was a toddler. A lot has changed since then and the science has become more mainstream but the job is still very rewarding.”
During those early days, embryology was still evolving and Adam saw the development of techniques such as the manipulation of sperm and eggs using a micropipette under a microscope, which is now a core skill for an embryologist.
These techniques, along with MicroTESE (a form of surgical sperm removal), are used to overcome the issue of male factor infertility and have given the chance of fatherhood to many patients.

Bourn Hall is still pioneering and its embryologists’ development of specialist IVF procedures have made these techniques accessible to many more patients.
“I think it’s important that we offer the full range of fertility treatments available,” says Adam, “as we can then give patients the best chance of success.
“Our understanding of the science has come a long way but the techniques developed by Steptoe, Edwards and Purdy are still widely used today,” he observes.
Pioneering embryologist
The clinic was one of the first to introduce blastocyst culture, which offers high rates of success. In this procedure, embryos are allowed to develop for up to five days in a Petri-dish before implantation, to ensure that cell division and growth is progressing and the embryos can reach the blastocyst stage. The embryologists monitor the progress carefully as not all embryos have the potential to reach the blastocyst stage, but when they do the chance of pregnancy is increased.
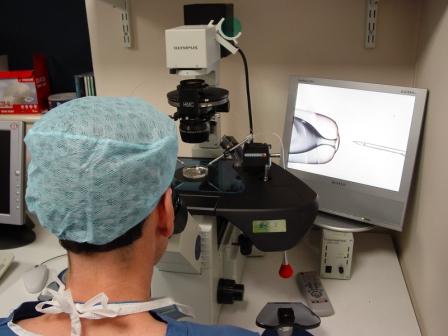
More recently it has extended this monitoring with the introduction of time-lapse technology. Adam observes: “Where previously embryos had to be removed from an incubator to be examined or graded, this is now no longer necessary as time-lapse technology and the capturing of images allows us to see embryos in situ, removing the need to disturb them, whilst also providing further insights into embryo development.”
Whilst the compulsory theoretical qualifications such as the STP is a prerequisite nowadays, Adam stresses that strong theoretical knowledge and good academic results, while important, don’t automatically make a good embryologist. “You need to have good manual dexterity and excellent eye-hand coordination,” he explains. “Spatial awareness is also crucial. We work as a team, and you can be sharing a small work-space with four or five other people.”
The closeness of the team is apparent as soon as you enter the embryology lab. “We have to work well together. Regulations dictate that every movement of eggs, sperm and embryo must be witnessed by a second qualified person, so we’re constantly calling on one another. Sharing information is crucial so getting on well with one another helps create a great team dynamic.”
Social skills, good knowledge and a confident manner when talking with patients are also very important. At Bourn Hall, there is an ever increasing amount of patient contact and embryologists are often called upon to explain procedures, discuss the benefits and risks of various treatment options and provide statistics and information which allow patients to make the best choices for them, as well as providing updates on embryo development when required. “It’s great to talk with our patients or meet them face to face,” smiles Adam. “Being able to put faces to the name on the dish adds a terrific personal element to what we do.
Frozen embryo treatment offers high success rates
Bourn Hall was one of the first clinics to freeze embryos that are of suitable quality and not transferred during the fresh treatment cycle. These can be stored for use if the patient needs a further cycle of treatment or perhaps to produce later siblings. The success rates for frozen embryo transfer (FET) have improved and are now comparable to a fresh cycle, leading to an increase in the number of successful cycles using frozen embryos.
The embryos are stored in huge vessels known as dewars – like giant thermos flasks full of liquid nitrogen. “You have to be an accurate record-keeper,” says Adam. “We have around 6,000 frozen embryos stored here, and we are able to locate any one of them in moments.” An ongoing programme of stringent monitoring ensures that every frozen embryo is safe, secure and accounted for, and the clinic is regularly inspected.
At busy times, Bourn Hall embryologists can help up to 50 patients a week. This means performing 10 egg collections and fertilisations per day. “You must work quickly, but very carefully whilst always being aware of the fact that you’re dealing with precious human embryos.”

Working at Bourn Hall has given Adam the chance to continue studying alongside his work – the clinic sponsored him through an MBA degree, and allowed him a sabbatical to travel in India.
“It’s a very rewarding job,” Adam concludes. “I still get enormous satisfaction from helping people become parents. Being able to do that in a friendly environment which encourages personal development is really all I could ask for.”







